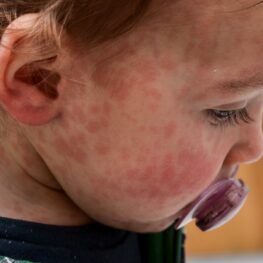
In recent months, there’s been a lot of discussion of Narcan, the drug that rapidly reverses opioid overdose whi, which the U.S. Food and Drug Administration approved for over-the-counter sale last March.
This month, the Washington legislature unanimously approved a bill requiring that every public school in the state have Narcan (naloxone) on-site in case of an overdose emergency. As of this writing, the non-partisan proposal only awaited Gov. Jay Inslee’s signature to become a law that goes into place June 1.
Should every parent keep Narcan (naloxone) in their medicine cabinet and a dose in their pocket – just in case? Should teens, even if they don’t use drugs, be taught how to administer the nasal pump and be encouraged to carry it? Would parents and teens carrying Naran help reverse the significant increase in drug-related teen deaths in King County in the past few years?
And that ever-present question of parenting: How do we keep our kids safe?
We brought these questions to Brad Finegood — a man who follows drug and overdose trends closely. Finegood is Public Health – Seattle & King County‘s strategic overdose prevention and response advisor. Moreover, he knows personally the grief of losing a loved one to overdose – his beloved brother died that way. And, perhaps most important, Finegood is a father. Here are Finegood’s thoughts:
Seattle’s Child (SC): Let’s start with the big question. Is the opioid, and in particular the fentanyl situation, in King County as bad as it sounds?
Brad Finegood: I don’t ever want to use scare tactics. We tried to use scare tactics in the old war on drugs days. I mean, I grew up with Nancy Reagan telling us our brains on drugs were like eggs sizzling in a frying pan and stuff like that. But that did not make me not want to use drugs. The truth is scare tactics don’t work.
What I will say is that fentanyl has really changed the game. One of the things that has changed is the risk perception. There are different forms of taking drugs into the body. For years and years and years and years, to get to a lethal amount of drug, (for the most part) someone needed to inject or inhale it. Today, you’ve got kids saying, ‘I’m never going to inject drugs!’ Like it’s a safety threshold, they won’t cross, so they’re safe.
The thing is, today, you don’t need a needle to use very lethal drugs. They are very cheap and very readily available. Without ever using needles, it’s easier to use a deadly drug than it ever was.
We might have had three fentanyl-related overdoses a year in King County in the past. This year, we’ve had well over 1,000 people die from fentanyl.
SC: How many of those are our kids under 18?
Finegood: From 2015 to 2018, we lost an average of three teens annually in King County. Last year, 21 teens died of overdose. So it’s happening with teenagers.

Image from StopOverdose.org
SC: You’re a parent. Narcan is now available over-the-counter. Do you have Narcan at home?
Finegood: As a parent, I decided it was in our best interest to stock Narcan/naloxone in the house once my kids were teenagers. At the floor level, it never hurts. It’s only going to hurt when you don’t have it when you need it and when you are least expecting it. In my work, I’ve talked to so many parents who had no idea that their kids were using substances — kids who weren’t addicted but were experimenting. Naloxone has no known adverse impacts if it is used on something other than an overdose. So it is extremely low risk.
One of the things about fentanyl coming into our community is that it comes in the form of a pill, and often, people have a lower perception of the risk with pills. As if because it’s in a pill form, it can’t be that unsafe. Again, it doesn’t require using a needle.
And I can’t tell you how many parents I’ve talked to after their kids have died who said, ‘If there’s one thing that I wish I would have done, it was to have naloxone in the house so I could have been able to respond.’
SC: Do you think all parents and teens should carry Narcan?
Finegood: I do. I carry it with me when I leave the house — not just for my family, but for anybody I might come in contact with who needs it. I think it should be part of the [family medicine cabinet ].
It’s always better to be safe than sorry. I know a lot of parents and teens that have Narcan on them. And I don’t know anyone who’s ever regretted having Narcan on them.
SC: What did you say to your teens when you decided to keep naloxone on hand and easily accessible?
Finegood: I’m really open with kids and interested in what they’re seeing, what they’re understanding, how they’re experiencing things, and talking through things. I said, ‘Hey, I care, and I will have this in the house. And I just want you to know, and I want you to feel comfortable with it. And I want you to know that this isn’t a judgment on you.’
My kids know my brother passed with an overdose and that I wouldn’t want this to happen to them or any of their friends. I told them if there’s ever a situation where we need it for them or a situation where they need it for any of their friends, here’s where it is.
My kids know people who are using substances are often struggling with some mental health concern and possibly even a diagnosis. I told them, ‘Having Narcan isn’t a judgment, it’s just a safety mechanism’ and ‘Please never hesitate to wake me up in the middle of the night or hesitate to ask me questions about it.’
SC: Should we teach all teens how to administer Narcan?
Finegood: My kids know how to use naloxone or Narcan and know what an overdose looks like. Because if I’m not home, I want to ensure everything’s okay.
It’s easy to use. Narcan is administered inter-nasally and is now available over the counter in most pharmacies. I’ve seen it at my local pharmacy; there’s a nice little stand with it.
I think it helps parents and teens to know that Narcan has no adverse side effects if it’s used on somebody who is not having an overdose. I think that’s important and makes people less fearful about using it. If I was sleeping hard and someone sprayed Narcan up my nose, there would be no positive or negative effect if I was not overdosing on opioids. There are just no negatives. It was also important to me that my kids know what an overdose looks like so that if they’re around their friends or in their community, they can respond.
Another essential thing is to make sure you and your kids know to call 911 when you feel an overdose is happening.
SC: How do you know if a person is overdosing rather than sleeping?
Finegood: We all should get educated about what substance use, especially fentanyl use, looks like. We need to know that when someone is extremely groggy or hard to wake up, overdose is a possibility. Of course, many teenagers are often hard to wake up. I go through that every single day in my house. But we are talking about a person who is abnormally hard to wake up, groggy, or sedated, (possibly snoring abnormally). It’s something to keep a look out for. From the lens of having a brother who died of an overdose, I can’t say enough how important it is to know what to look for and how to respond.
My younger brother was my best friend, and yet we didn’t know he had substance use problems. The day he overdosed, he showed all of the signs that he was experiencing an overdose, but the people with him that day decided to let him go back to sleep to sleep it off.
SC: You shouldn’t let someone who seems to be sleeping unusually hard sleep it off?
Finegood: I can’t tell you how many parents thought that was the right idea for their kids. And unfortunately, they never woke up. If you suspect an overdose, don’t let them ‘sleep it off.’
SC: I was shocked to learn both of my kids tried several drugs in high school – not just the marijuana I assumed they would. Am I alone, or was I remarkably naive?
Finegood:That’s why it’s so critical that we, as parents, have constructive conversations with our kids about substance use in a non-judgmental way. I remember when fentanyl first came into our community. It was new to me, and I went to my oldest child and asked, ‘Hey, what do you know about this?’
Because I approached with curiosity, openness, and no judgment, he showed me his phone where the topic came up in Snapchat after Snapchat after Snapchat.
Kids know more than we expect and often more than we do. And so we can’t lead with judgment, we can’t lead with, ‘If you ever use, I’m going to shut your computer off or take your phone away’ or stuff like that. You need always trying to figure out ways to keep that line of communication open so your kid feels safe and comfortable talking to you about what they’re experiencing and seeing. They don’t want that shame or stigma put on them.
The other thing we know is that, almost undoubtedly, whether kids are experimenting or not experimenting, they often know kids who are. And they tell us they want to be equipped to help the struggling people they know.
SC: Did you, and should other parents, teach their kids how to administer Narcan?
Finegood: My kids know how to use naloxone/Narcan and know what an overdose looks like. Because if I’m not home, I want to ensure everything’s okay.
Over-the-counter Narcan is not hard to use. It’s an inter-nasal spray and is now available in most pharmacies; I’ve seen it at my local pharmacy, and there’s a nice little stand with it.
Parents and kids need to understand that there are no negative side effects if Narcan is used on somebody who is not having an overdose. If I was sleeping really hard and someone thought something was going on and sprayed Narcan up my nose, there would be no positive or negative effect unless I was overdosing on opioids.
But make sure you and your kids know to call 911 when you think an overdose is happening.

Poster provided by Public Health Seattle-King County
SC: What does an overdose look like?
Finegood: It looks like somebody who’s really overly tired, overly sedated. If you can wake somebody up, they don’t need Narcan. But it’s also critical that you don’t let them go back to sleep. Public Health Seattle-King County has some great posters with visual graphics that help identify overdoses. But it’s really like an oversaturation. It’s a sleep so deep that the person’s respiration goes down so much that they stop breathing.
If you think somebody’s overdosing, the best thing you can do is ask them if they’re okay. I do this, actually, on a fairly regular basis. If I’m out in the community, and I see somebody who looks like they’re falling asleep in an irregular position, sort of a forward-facing slouch, I will stop and ask, ‘Hey, are you okay? Hey, are you okay?’ then raising the voice slightly more.
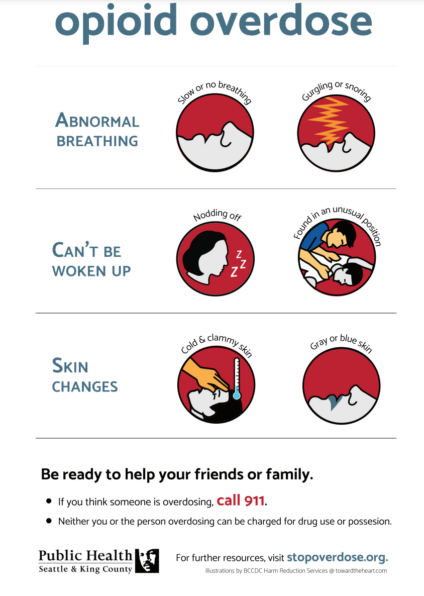
Poster provided by Public Health Seattle-King County
SC: What do you say to parents who fear having Narcan in the home or carrying it or giving it to teens to carry is, in essence, telling their kids they condone drug use?
Finegood: We teach our kids from an early age about safe sex practices. That doesn’t necessarily condone them having early sex.
The truth is that even if they aren’t experimenting, kids care about other kids. And being able to be responsive in those overdose situations is important to them. If we, as parents, deny their truth, we’re pushing them further away. I talked to my kids about drugs all the time. But part of it is because of what I do. But part of it is because I feel like I’m a responsible parent.
My kids, to the best of my knowledge, have never tried opioids, but they know what an opioid is. They know what fentanyl is. And they know how to respond to an overdose.
SC: Is there any good news when it comes to the opioid crisis?
Finegood: It’s not all doom and gloom. So far, in 2023, 16 teens have died, 15 confirmed and one suspected.
It’s clear there’s experimentation, and we want people to be hyper-aware of that and to ensure teens and parents are educated. For those teenagers who are truly addicted and are having trouble stopping, we have effective medications that help manage cravings – like buprenorphine. If you are over 16, you can get it by visiting your doctor.
SC: Are there things that increase the risk that a young person will overdose?
Finegood: It’s a common misperception that just telling kids to stop using or to get it together and be abstinent will keep them from using. But it can stop them from getting the support they need. They might stop for a while but then go back to it. One of the things that happens is when people stop using, their tolerance goes down. If they slip up and go back to using when their tolerance is down, their overdose risk rate goes up. That’s how my brother died.
That’s why medications like buprenorphine help can make such a difference when it comes to overdose risk.
SC: Are there other misconceptions you think parents should know about?
Finegood: Yes. I guess this is on the positive side. There’s a widespread misperception that’s been perpetuated by the media and on social media that fentanyl is in ‘everything.’ I’ve heard it from my friends. I hear from doctors. But the truth is fentanyl is not hitting everything (in terms of drugs teens may be trying). One of the places we have not seen it is in marijuana.
There’s a lot of misperception out there that fentanyl is like in marijuana pens and laced in all the marijuana. The truth is marijuana bought from the store is highly regulated and controlled. Public Health keeps a watchful eye on what’s happening in the community — our surveillance is extremely strong here. And if we do see fentanyl in marijuana, we will make sure to get the word out on it.
But we have not seen it at all, despite what’s been reported.
SC: Anything else you’d like to say to parents?
Finegood: I just want to say it again: I have never met a parent who was sad that they had a conversation with their kid. I’ve only met parents who were sad that they didn’t have a conversation with their kid.
Read more: